Ann Geier, MS, RN, CNOR(E), CASC, is the chief nursing officer for Surgical Information Systems. She has worked in the ASC industry for more than 30 years and has been responsible for every aspect of ASC financial and clinical operations.
In addition, Geier is a surveyor for the Accreditation Association for Ambulatory Health Care (AAAHC) and serves as the secretary/treasurer for the Board of Ambulatory Surgery Certification (BASC). BASC is the organization that administers the Certified Ambulatory Infection Preventionist (CAIP) and Certified Administrator Surgery Center (CASC) exam. Geier recently helped develop the CAIP exam, which was first administered in October 2018.
In this article, she discusses five issues concerning ASC infection prevention.
On the Role of the ASC Infection Preventionist
Ann Geier: ASCs are mandated to appoint an infection preventionist (IP), but most people who assume this role are not adequately prepared to fill it. In some instances, someone on the ASC's staff will volunteer for the position, but it's often a "tag, you're it" role — an individual happens to be in the "right" place at the "right" time to fill the position, even if they do not necessarily want it.
Regardless of how one assumes the role, the key to serving as a good IP starts with adequate training. Then it's all about dedication to the position and its responsibilities, as well having the time to perform the work one must complete. That is typically anywhere from 2-8 hours each week, although some IPs spend more time fulfilling their responsibilities.
Regardless of whether you're on the low or high end of that time allocation, what matters, as noted, is having dedicated time to complete infection prevention work. This sometimes will need to be ramped up. For example, if an infection requires investigation, the IP needs the ability to perform a complete investigation.
IPs must also be prepared to periodically play the "bad guy." If an IP performs an audit and finds a problem, they must be able to call out the responsible parties and explain that these individuals are not following proper policies and procedures.
On the Value of CAIP Certification
AG: We came up with the CAIP certification to serve as a form of recognition for those ASC professionals who put in the time to learn how to effectively serve as ASC IPs. We wanted to offer the opportunity for these professionals to achieve another level of credibility — to earn a "Good Housekeeping seal of approval," if you will.
The process of working toward and maintaining certification keeps you motivated and learning. Furthermore, earning CAIP provides you with an extra credential that you can utilize to your advantage. It's what I call a "marketable skill." If an IP holding the CAIP credential decides to move on from their current position, ASCs considering hiring that IP know the professional has put in the work to become a good ASC IP.
On the Importance of an ASC Infection Prevention Risk Assessment
AG: The risk assessment is where ASC infection prevention should start. The Centers for Medicare & Medicaid Services (CMS) mandates that ASCs perform an infection prevention risk assessment. IPs are expected to develop that risk assessment. Fortunately, there are numerous tools available from different sources that can help guide in developing the assessment.
These sources can provide a helpful template, but the key to the risk assessment is then configuring and personalizing it for your particular center. For example, if your ASC is in Oklahoma, one of the risks you will want to take into consideration is the high probability of tornados. You would want to ask yourself, "What does this do to my infection program?" If you're in South Florida and have migrant workers in your community, what does that do to your program? There are a lot of consequences to both of these examples. Every ASC has important considerations like these. You will need to figure them out as part of your assessment.
After you have completed the risk assessment, your work must be prioritized. Up first: determining what's your greatest risk of infection and what's your greatest vulnerability.
On Problematic ASC Infection Prevention Areas
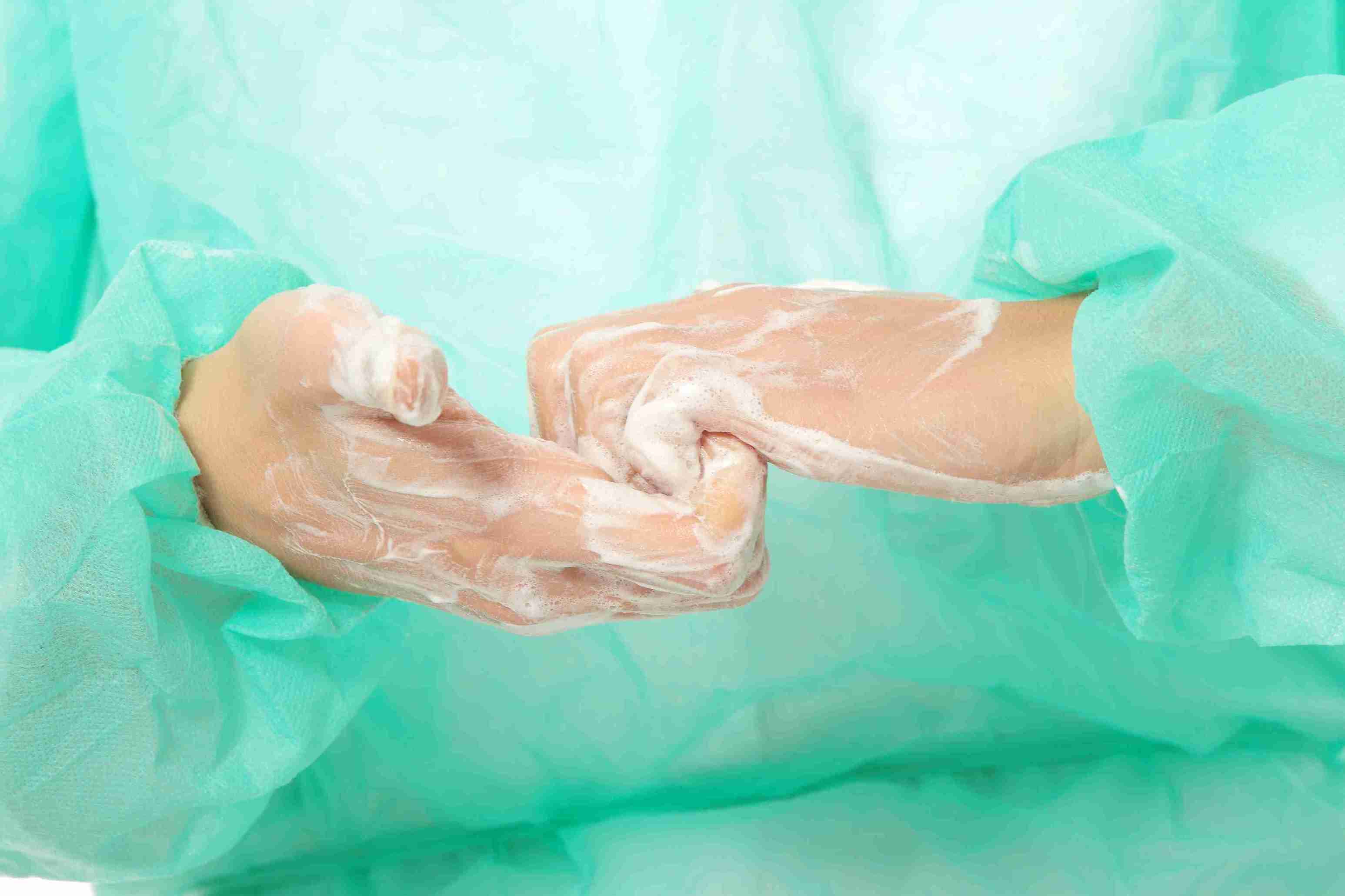
AG: Hand hygiene is always near the top. The reason: People are people. When one is appointed the IP, you usually watch your staff like a hawk at the start. If everything looks good, it's only natural to take your eyes off the staff for a bit. After all, an IP has lots of other responsibilities. But this leads to people getting comfortable in their work environment, so they slack off a bit. It's human nature.
Further complicating matters is when you add new staff and have outside practitioners coming in who perhaps do not take infection prevention as seriously as you do. Hand hygiene is one of the simplest, most important, and yet still challenge areas of infection prevention.
Safe medication practices remain a problematic area for many ASCs. People still cut corners on these practices, such as by not wiping the stoppers on multi-dose dials or performing two-handed recapping. Any time a corner is cut, patient and employee safety is at risk.
The final area I want to highlight is sterilization. The key question IPs must answer is, "Is your ASC completing every step in the sterilization process as instructions for use (IFUs) require?" You should never perform sterilization from memory. Also, understand that sterilization is not an area that someone who lacks adequate training should be working in. There's too much risk for error.
These are three areas we look at closely as surveyors and are areas IPs should zero in on.
On Governing Body Support
AG: The governing body should appoint the IP and this appointment should be documented in the governing body minutes. Then the governing body must support the IP going forward for the IP to succeed in the role. The governing body should allocate the time required to complete the work an IP must do. An IP should also be allowed — and encouraged — to pursue educational and training opportunities (e.g., conferences, webinars, online courses).
If there's an investigation that's required, the governing body must have the IP's back, supporting completion of the root-cause analysis. A governing body should never try to stop the investigation. The governing body must respect the investigation report, even if they disagree with it. You can always have a reasonable back-and-forth discussion about the findings.
Finally, the governing body should let everyone on the ASC's staff know that the IP is an essential position that deserves respect and has the governing's body unwavering support.
Geier will be presenting a webinar on "Taking the Infection Preventionist Seriously" on August 6 at 1:00 pm ET for the Ambulatory Surgery Center Association. Learn more and register.