While operating rooms are critical for patient care, they are also important to a hospital’s profitability as the OR is known as a key revenue generator in any facility. Where is the potential to optimize the OR’s revenue? The answer lies in factors like case scheduling, resource allocation, supply costs, and other key performance indicators for surgery-specific metrics. Data can reveal needed process improvements related to these types of case flow and business needs. These opportunities can bring about both increased revenue and decreased costs.
The following tips will help you take advantage of operating room analytics and established approaches to operational efficiency so your OR can see greater profitability per procedure and overall financial success.
- STAY ENGAGED
If you want to enact changes in the OR, you need support from those involved in the process, especially physicians. The best way to get their active, visible assistance is to engage them. Encourage their participation in addressing process improvements rather than merely telling them what to do. Physicians are at the core of much of the work done within the operating room, so they have unique insight into operational practices and can be great resources in figuring out how to make things better. Empower them to get involved, and you will likely see more buy-in when it comes to embracing change.
However, process improvements do not just require engagement from leadership. You will want to engage the entire team. It can help to think of your organization as a larger universe that is made up of a bunch of microsystems or small groups of providers and staff that work together to deliver care. Boil the process down to the smallest units of care activity and work to refine the processes within them.
- MEASURE APPROPRIATELY
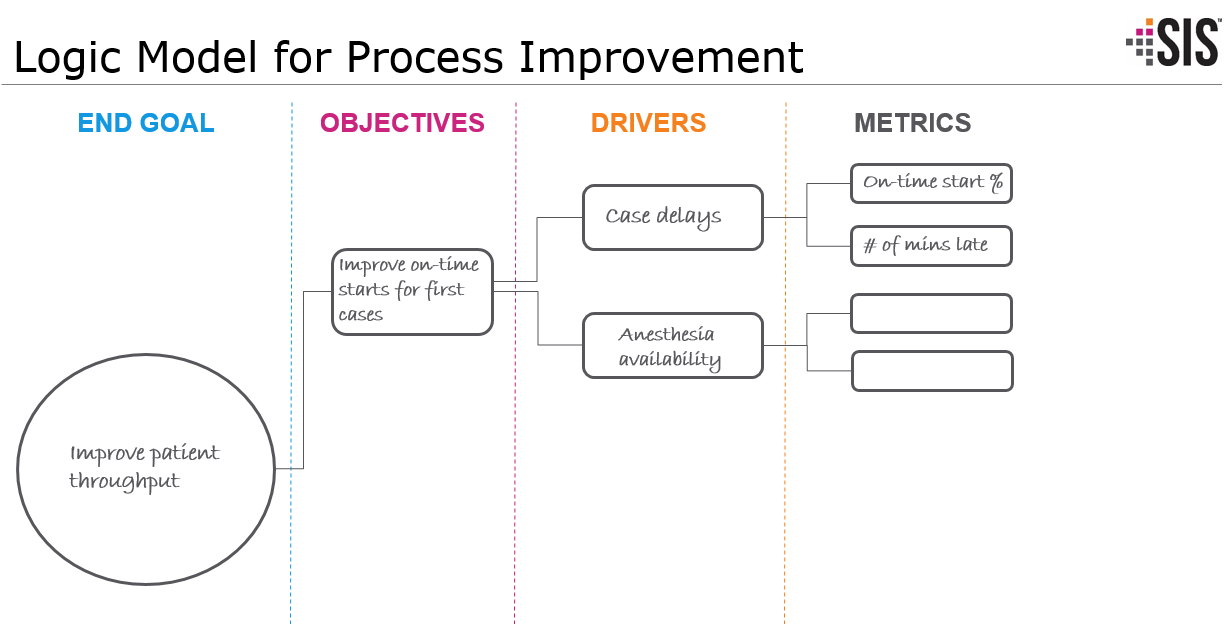
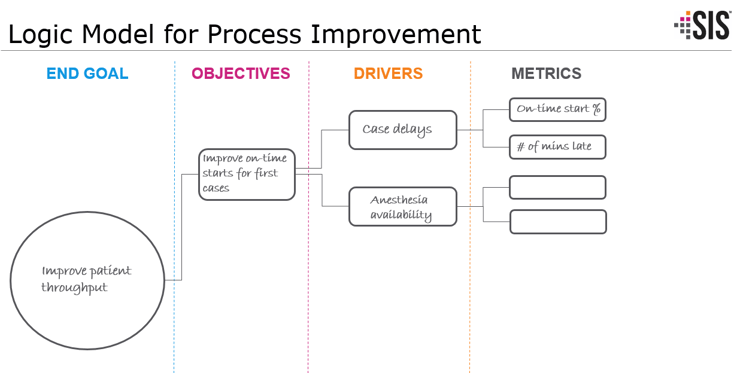
Process improvement in the OR is data-driven. You have to be able to measure performance in order to effectively gauge progress. But what and how do you know what to measure? We work with a logic model process that looks at the end goal, objectives, drivers and metrics. Start with your end goal (improvement in patient throughput, for example) to define your objective(s) — in this case, improved on-time first case starts and decreased latent time. Then, decide on the drivers you want to focus on to achieve those objectives, and specify metrics that are indicators of the drivers. To improve on-time first case starts, for example, you need to track case delays, ensure anesthesia availability, and provide patients with the appropriate information for arrival.
SIS Analytics is a useful tool for capturing your data and analyzing individual metrics in the perioperative environment. The tool helps facilities see a clear view of their operations, identify opportunities for improvement, and monitor progress.
- CELEBRATE SUCCESS
No matter how big or small the initiative, find a way to celebrate success. It will not only help recognize those involved, but also it can promote a culture of innovation and encourage future efforts for quality improvement. This does not have to be fancy; it can be as simple as hanging a sign of recognition on the bulletin board or it can go as far as to provide a bonus incentive. Be sure to spread the word by taking advantage of your center’s various communication outlets (emails, newsletters, websites, social media) to let everyone know the good news, especially if the change you are making offers benefits to patients.